Meet Our Doctor
Dr. Paresh Bang

Stitchless Spine Surgery In Nagpur
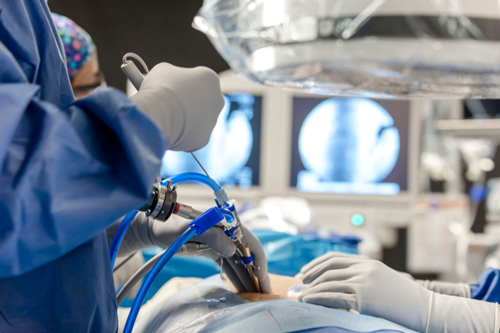
Minimally invasive spine surgery, often referred to as stitchless spine surgery, is an advanced surgical technique characterized by smaller incisions and the utilization of specialized instruments. This approach minimizes tissue disruption and scarring when compared to conventional open surgery methods.
During Stitchless spine surgery, the surgeon employs specific instruments and techniques to access the spine through incisions typically measuring less than one inch in length. This strategy aims to reduce damage to surrounding tissues and muscles, resulting in benefits such as diminished pain, reduced blood loss, and a shorter recovery period in contrast to traditional open surgery.
Stitchless spine surgery for patients with spinal conditions
Nowadays, minimally invasive surgeries are increasingly favored by patients due to their numerous advantages. These procedures involve small incisions, unlike traditional open surgeries, specifically targeting conditions within the spine. Before such surgeries, anesthesia is administered to numb patients, ensuring they experience no pain during the procedure. Conditions like disc herniation, fractures, degenerative disc disease, infection, tumors, and instability are effectively addressed through these minimally invasive spinal surgeries.
The appeal of these surgeries extends to several key benefits. Unlike traditional open surgeries, which often require strict hospitalization and lengthy recovery periods, minimally invasive procedures offer quicker recuperation, minimal blood loss, and reduced pain and scarring.
Patients experiencing back pain and sciatica can find relief through spinal surgeries that do not involve stitches. One example is PELD (percutaneous endoscopic lumbar discectomy), a minimally invasive procedure that eliminates the need for stitches, pain, or muscle cutting during surgery. Conducted under local anesthesia, PELD is utilized to treat conditions such as herniated discs, low back pain, sciatica, and slipped discs.
